White Paper
The Need
For Speed
How Telemedicine Enables Faster Care in Rural Settings
The Problem
Patients present to rural emergency departments with emergent cases requiring immediate and timely attention and care teams must rush to meet important benchmarks to ensure quality health outcomes. Often times, local clinicians understand that time is of the essence and recognize the importance of established benchmarks but are often unprepared to meet these goals in a consistent fashion. This is not a reflection on the commitment, skill, or training these clinicians possess, it is simply a matter of available resources and staffing support.
The Question
How can we begin to start closing these gaps between actual care times and the benchmarks set forth by the Center of Medicare and Medicaid Services?
Dr. Katie DeJong, Avel’s Medical Director of Emergency, sought to help answer this question by spearheading an internal research study examining two common instances where timely treatment is essential: myocardial infarctions (heart attacks) and strokes. By analyzing the data available, Dr. DeJong’s team has come to a fascinating conclusion that reinforces the impact telemedicine has on rural hospitals, care teams, and communities.
The Solution
The telemedicine emergency quality data from Avel eCare’s thousands of patient interactions clearly demonstrates facilities who have telemedicine capabilities greatly benefit by engaging those services sooner and more regularly.
In the case of Avel eCare, the sooner hospitals and clinics engaged the services of eCare experts, the faster local care teams could diagnose heath emergencies and begin treatment. And, in the case of strokes and heart attacks, there is unmistakable evidence to demonstrate that telemedicine can help originating sites meet or even beat established benchmarks. This results in billions of cells, neurons and synapses preserved which, equates to saved lives.
Time is Muscle
For heart attacks – specifically ST-Elevation Myocardial Infarction (STEMI) — the time to fibrinolytics has been established as a reliable predictor of outcome for affected patients. Since nearly two lives per 1,000 patients are lost per hour of delay, national guidelines recommend that fibrinolytics be given to eligible patients within 30 minutes of arrival (1). This is a short window.
The Impact of Telemedicine
The process to diagnose and treat STEMI patients in emergency departments and achieve the goal of door-to-needle time of 30 minutes for thrombolysis is well documented, yet often difficult to achieve. To assess the impact of telemedicine on treating heart attacks in rural settings, Dr. DeJong and her team analyzed three metrics related to the diagnosis and treatment of heart attacks when eCare was engaged, including median time to EKG, fibrinolytic compliance for STEMI patients, and median time to fibrinolytics for STEMI patients
According to the clinical data, which was captured during the span of April to October of 2021, Avel’s telemedicine services help care teams request and interpret EKGs essentially within 6 minutes. This is roughly 4 minutes below the benchmark established by the American Heart Association (See Figure 1).
Ordering the EKG is only the first step. Next, the patient must be carefully screened to determine whether they should be administered fibrinolytics. This decision should not be made lightly – with the administration of these drugs comes the potential for serious adverse events including internal bleeding. When Avel’s telemedicine experts were engaged, they helped facilities ensure a 97.5% rate of compliance for fibrinolysis. The timelier and more accurate the diagnoses, the sooner eligible patients can receive the important clot-busting medicine. This is reflected in the median time to fibrinolytics for STEMI patients when Avel was engaged. On average, Avel helped sites meet a median FIB time of 33 minutes once the telemedicine service was engaged. As figure 3 illustrates, the sooner a site requested telemedicine support, the sooner they were able to administer fibrinolytics.
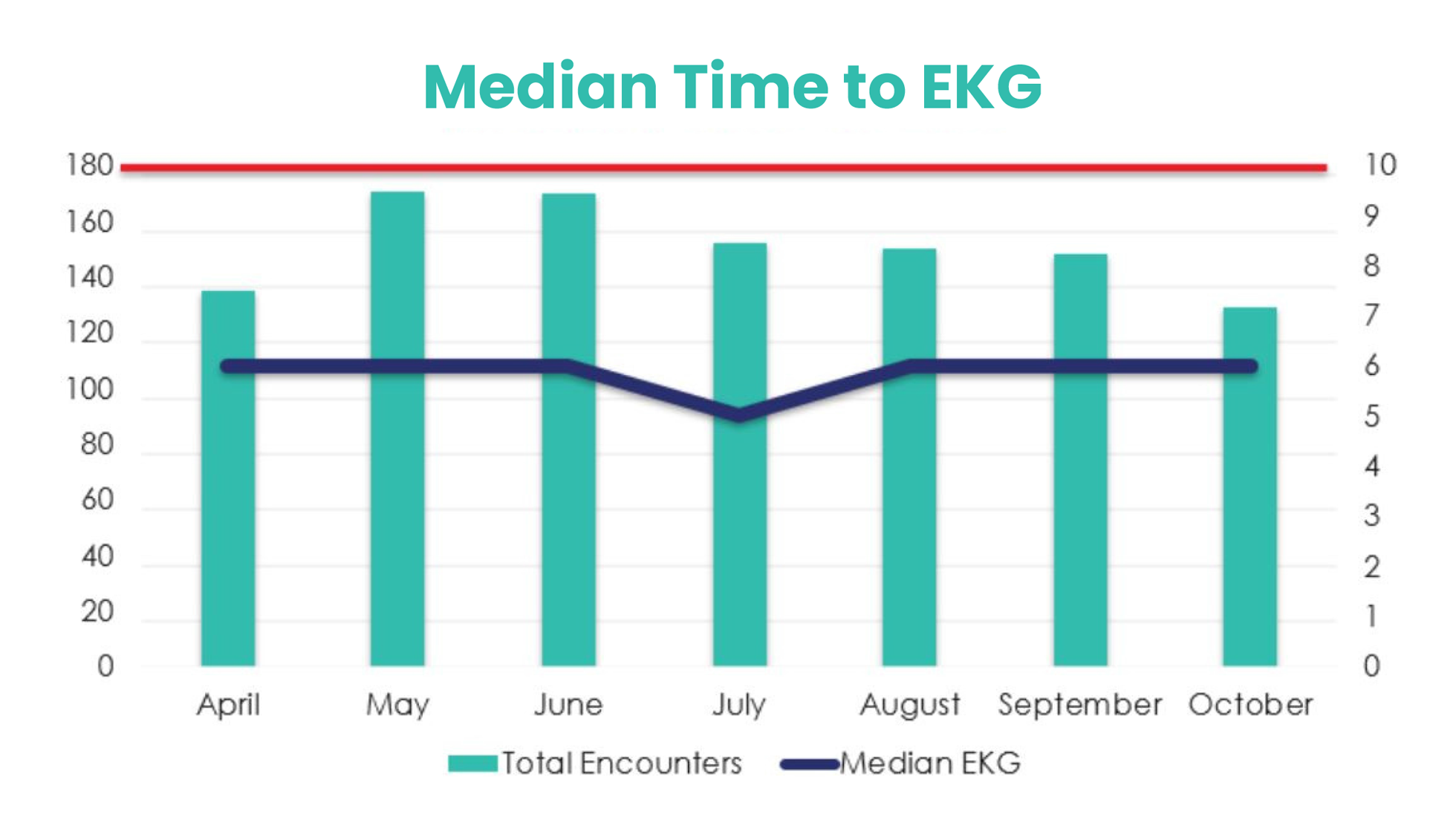
Figure 1: Avel eCare Emergency has a median time to EKG of 7 minutes or less during the past five years
On average, Avel helped sites meet a median FIB time of 33 minutes once the telemedicine service was engaged.
This is approximately 15 minutes sooner than the average for rural hospitals without telemedicine support, according to a recent study.
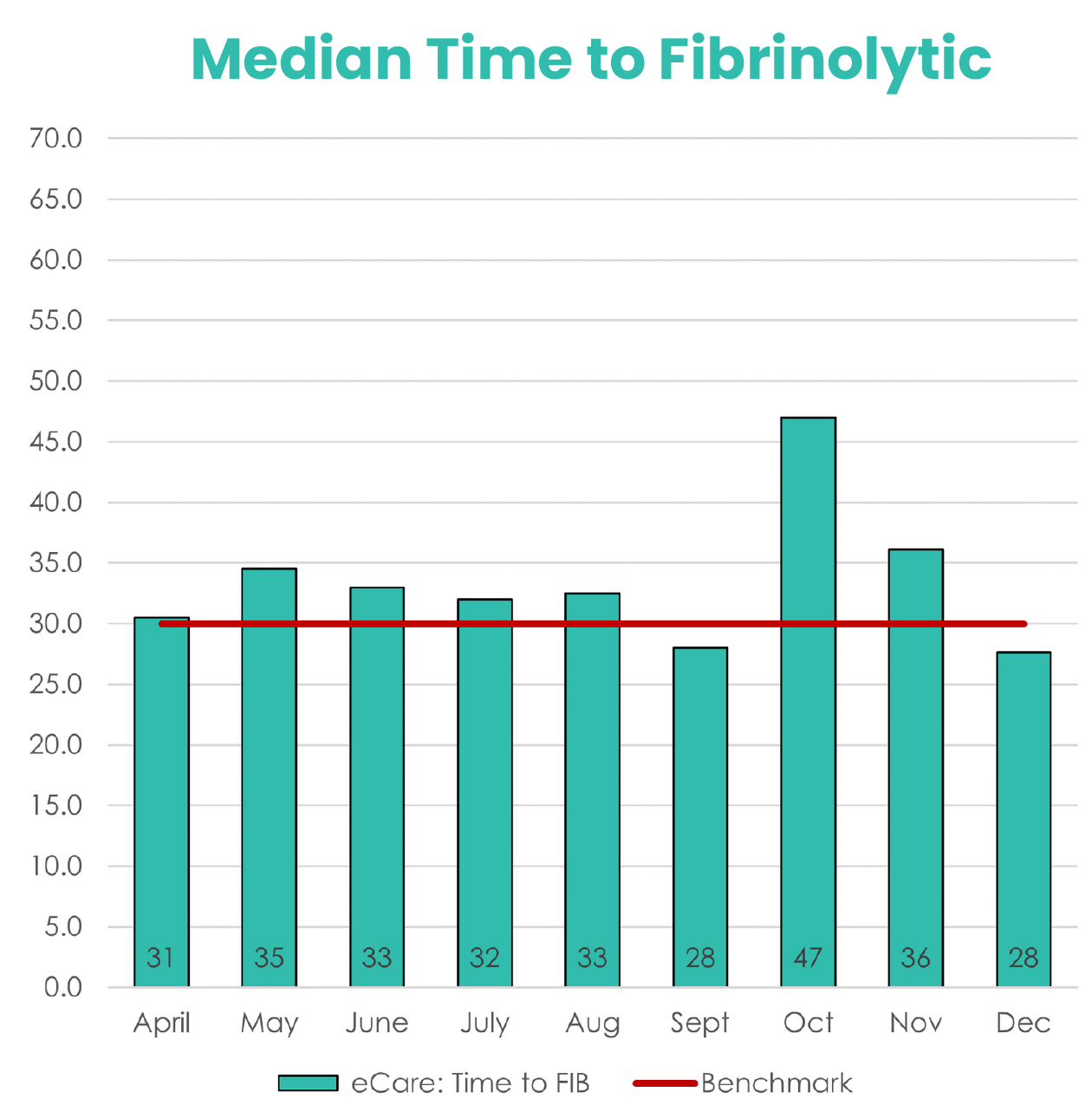
Figure 2
Time is Brain
Similar to heart attacks, blockages caused by a stroke can result in catastrophic outcomes and must be treated as quickly as possible. The quality benchmark that has been established to treat strokes is for patients to receive intravenous tissue plasminogen activator (tPA) in 60 minutes or less from when the patient arrives at a facility, when appropriate.
Pathway to Treatment
To utilize tPA, a strict process must be followed to administer this effective yet dangerous medication, including identifying the appropriate symptoms, performing and interpreting a CT scan, and screening for the tPA inclusion and exclusion criteria. In rural emergency departments with limited staff and resources, each one of these steps shrink the already tight time to tPA benchmark window. When every second counts, these facilities need every advantage to help their patients receive treatment.
How Telemedicine Can Help
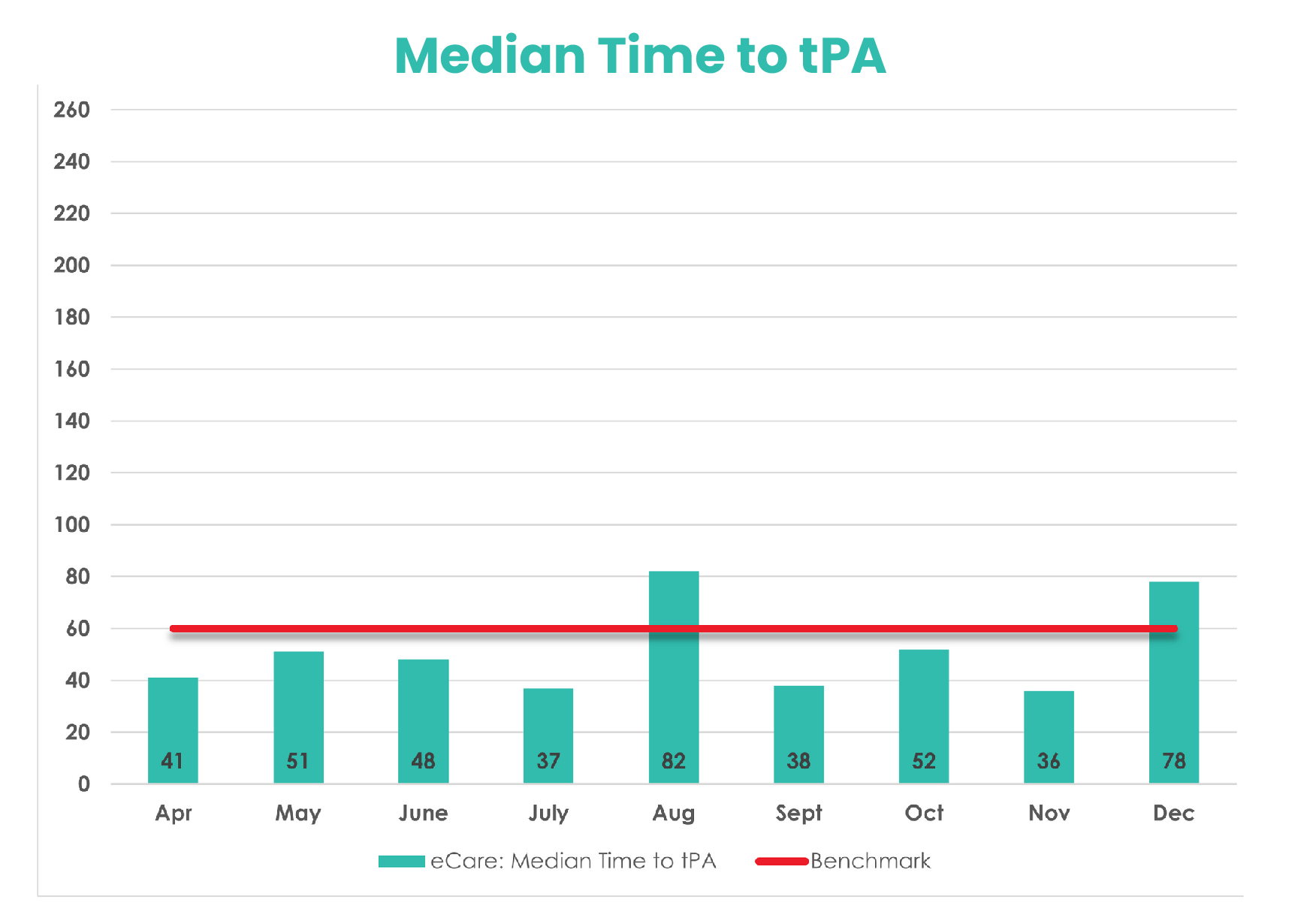
When eCare was engaged during the months of April through October of 2021, tPA was administered to eligible patients at a median of 51.5 minutes, nearly 9 minutes sooner than the benchmark of 60 minutes. These findings demonstrate how Avel’s assistance with stroke care improves administration of tPA and supports the bedside team in critical care. Notably, 100% of patients that should have received tPA received treatment when an Avel board-certified emergency medicine physician was involved in care.
Bottom Line: We’re Here to Help
Telemedicine can have a direct and positive impact on quality outcomes for patients. The sooner hospitals and originating sites initiate services with Avel eCare, the better they are able to meet established benchmarks related to stroke and cardiac care. When patient health and wellbeing is at stake, the added minutes and time saved for rural physicians, providers, and clinicians, is a gamechanger for rural medicine.